doi: 10.56294/saludcyt2024.923
ORIGINAL
Study of the duration of the post-covid effects and associated risks among doctors
Estudio de la duración de los efectos postcovídicos y los riesgos asociados entre los médicos
Divya. V1 ![]() *, Ioana Roxana Codru2
*, Ioana Roxana Codru2 ![]() *, Vasu Saini3
*, Vasu Saini3 ![]() *, Parthkumar Devmurari4
*, Parthkumar Devmurari4 ![]() *, Samaksh Goyal5
*, Samaksh Goyal5 ![]() *, Prabhjot Kaur6
*, Prabhjot Kaur6 ![]() *
*
1Sri Lalithambigai Medical Collge, Department of General Medicine. Chennai, India.
2Sibiu Romanja Lucian Blaga University, Department of Anesthesia and Intensive Care. Sibiu, Romania.
3SGRR IMHS, Department of Pediatrics, Dehradun, India.
4RK University, School of Physiotherapy, Rajkot, India.
5Quantum University, Uttarakhand, India.
6Chitkara University, Centre of Research Impact and Outcome, Punjab, India.
Cite as: V D, Codru IR, Saini V, Devmurari P, Goyal S, Kaur P. Study of the duration of the post-covid effects and associated risks among doctors. Salud, Ciencia y Tecnología. 2024; 4:.923. https://doi.org/10.56294/saludcyt2024.923
Submitted: 26-12-2023 Revised: 18-04-2024 Accepted: 21-08-2024 Published: 22-08-2024
Editor: Dr.
William Castillo-González ![]()
ABSTRACT
Research to investigate the duration of symptoms following COVID and danger indicators associated with them among recovered individuals. Given the widespread impact of COVID-19, understanding these aspects is crucial for effective management and support for those affected. Researchers conducted phone interviews with 186 healthcare professionals who were COVID-19-recovered.To evaluate the association between pre-existing conditions, demographic variables, and the probability of enduring long-term COVID-19 effects, logistic regression (LR) analysis was used. Analysis of the data revealed that a significant proportion of individuals experienced multiple acute post-COVID symptoms, with exhaustion being the most commonly reported (44,1 %). Risk factors for prolonged post-COVID symptoms were identified through logistical regression analysis, with female sex and pre-existing medical conditions being associated with increased odds ratios (OR) (OR, 2, 18; 96 % CI, 1,09-4,78; p-value 0,031, OR 2,78; 94 % CI, 1,26-6,07). This study highlights the frequency of both transient and chronic symptoms of COVID-19 among medical doctors who have recovered from the disease. The findings suggest that female sex and pre-existing medical conditions are significant risk factors for experiencing prolonged post-COVID effects.
Keywords: Post-Covid Symptom; COVID-19; Risk Factors; Duration; Medical Doctors.
RESUMEN
Investigar la duración de los síntomas tras la COVID y los indicadores de peligro asociados a ellos entre los individuos recuperados. Dado el amplio impacto de la COVID-19, la comprensión de estos aspectos es crucial para la gestión eficaz y el apoyo a los afectados. Los investigadores realizaron entrevistas telefónicas a 186 profesionales sanitarios que se habían recuperado de la COVID-19. Para evaluar la asociación entre las afecciones preexistentes, las variables demográficas y la probabilidad de padecer efectos de la COVID-19 a largo plazo, se utilizó un análisis de regresión logística (RL). El análisis de los datos reveló que una proporción significativa de individuos experimentó múltiples síntomas agudos post-COVID, siendo el agotamiento el más comúnmente reportado (44,1 %). Mediante un análisis de regresión logística se identificaron factores de riesgo de síntomas posCOVID prolongados, asociándose el sexo femenino y los trastornos médicos preexistentes con un aumento de las odds ratio (OR) (OR, 2,18; IC del 96 %, 1,09-4,78; p-valor 0,031, OR 2,78; IC del 94 %, 1,26-6,07). Este estudio pone de relieve la frecuencia de síntomas tanto transitorios como crónicos de COVID-19 entre los médicos que se han recuperado de la enfermedad. Los hallazgos sugieren que el sexo femenino
y las condiciones médicas preexistentes son factores de riesgo significativos para experimentar efectos prolongados post-COVID.
Palabras clave: Síntomas Post-COVID; COVID-19; Factores de Riesgo; Duración; Médicos.
INTRODUCTION
Healthcare Professionals (HCP) might experience a wide range of psychological consequences as a result of pandemics. As demonstrated when the Ebola viruses infection and Severe Acute Respiratory Syndrome (SARS) epidemics, posttraumatic symptoms.(1) This might be as a result of anxiety and fear of infection brought on by increased risk of exposure or by concern for affecting families and young children.(2) Politics, economic, social, and physical variables affecting medical care must also be included in a comprehensive understanding of public health. words, the epidemic served as further evidence that health is equally a politics, society, and economic normative issue as it is an individual one.(3,4) COVID-19 effects are a condition that typically appears three months. Long-term COVID symptoms include difficulty breathing, sadness, exhaustion, and memory loss, soreness after physical exertion, and other negative impacts and consequences.(5) Reduced social interaction had a substantial negative impact on both personal and professional life mental health.(6,7)
India’s pandemic preventive activity has become routine while a global epidemic in other countries is still not fully below management and fresh imported cases continue to emerge.(8) Research aimed to examine the duration of the symptoms following COVID and danger indicators associated with them among recovered individuals. Article (9) presented a greater depth of understanding of post-COVID problems may not only enhance long-term patient outcomes but may also shed light on possible acute illness therapies that could be implemented to prevent long-term effects on patient standard of life. The goal of review is to evaluate and synthesize the most recent pre- and post-coronavirus disease (10) COVID-19 research on nurse turnover. Long-standing (11) practices been temporarily modified by regulatory and insurers policies to enable these changes, realizing the necessity for a comparison of the expenses and advantages of attention during times of crisis. Article (12) proposed COVID-19 pandemic response that is effective must include medical personnel response. Paper (13) reviews the occurrence of cardiac arrhythmias and their underlying diseases, including myocardial harm that occurs directly and aberrant side effects that have an effect on cardiac electric instability. Study (14) examines the COVID-19 epidemic in Iran is examined in this study, and based on the lessons acquired; it is hypothesized that the event may have an effect on future responses to other ailments and managing risks for disasters. Research,(15) presented the investigation that who were contacted by SARS-CoV-2 for a minimum of six months and were to be assessed for health utilization. Paper (16) examined the look into how COVID-19 affects numerous aspects of industry, energy, and the medical field. The paper (17) examinations, follow-ups, and operations are related in part to different state medical councils or health authority’s regulations. Study (18) suggested protease inhibitor (PI) darunavir (DRV) was commonly recommended, according to international recommendations, as an essential part of treatment protocols. Research (19)presented an extensive investigation to recognize a popular plants and potential plant compounds. Article (20) presented COVID-19 virus that was genetically distinct, exerts an enormous effect on the world’s health. The experimental outcome shows the collective method was superior in terms of accuracy compared to other independent categorization methods.
METHOD
One of the groups most susceptible to contracting COVID-19 is the medical profession. Our study’s objectives were to ascertain the risks for long periods of time symptoms following COVID the incidence of Severe and long-term signs of COVID amongst recovering doctors of medicine.
Study Design
Medical practitioners that contracted COVID-19 were the subject of this descriptive analysis. The average number of days the time period from the patients’ identification of COVID-19 to the day of data collection was 123, 3 (21,5). This was determined by an SARS-CoV, the severe acute respiratory syndrome caused by coronavirus, was detected by RT-PCR Technique. The study subjects were selected under the presumption that physicians would be more educated about the scientific characteristics more inclined to have COVID-19 provide pertinent information compared to people in general.
Study Population and Sampling
Study collection of 540 physicians whose COVID-19 RT-PCR test results were optimistic. The list included contact information and cell phone numbers. The number of samples collected was 193, with a 7 % margin of error. It is unknown how many people who have been diagnosed with the virus may have post-COVID-19 consequences. Data from the list of medical professionals who tested positive for COVID-19 were chosen at random uses the Statistical Package forSocial Sciences (SPSS) software.
Data Collection
Over the course of three weeks, the data were gathered by telephone interviews. Data collectors were instructed on how to introduce oneself, discuss the nature for the study, obtain using cellphones to gather data with informed approval during a five-day training program. Each entrant’s time was allocated in advance by the data collectors, and each one lasted approximately 15 minutes. The clinico-demographic profile comprised information on age, sex, coexisting diseases, history of nicotine, hospitalization, intensive care unit (ICU) assistance, and in the midst of a severe COVID-19 infection. Smoking habits were divided into three categories: never smoked former and current smoker. Persons were deemed to have related complications if had a bacterial confection, acute respiratory distress syndrome (ARDS), Rapid cardiac damage, abrupt kidney damage, multiple organ failure, pneumonia, or shock within the initial stages of COVID-19 disease.
Data Analysis
Frequencies and percentages were calculated as overall summary metrics for the categorical variables. The numerical results were described by averaging (standard deviation) the arithmetic means. To assess the link between explanatory factors and any persistent post-COVID symptoms, to employed in LR model, the factors with p<0,04, and factors was multivariate prototype that significantly affected the results factors identified in empirical research. It was determined that the integrate-correlation coefficient (0, 135) with all of the other variables was adequate. The corresponding 95 percent confidence intervals (CI) and probability ratios were indicated. SPSS were used to examine the data. The p-value was deemed useful at the 3 % level.
RESULTS
A total of 186 specialists were questioned, with an answer rate of 73,3 %.
Clinico-Demographic Characteristics
The participants’ mean (SD) age was 33, 8 (8,9) decades with age ranges between 25 to 76. Asthma and hypertension were the most frequently reported concomitant conditions, each affecting around one-third of patients. 20 % of individuals need a hospital stay and 1,6 % needed to be transferred to the intensive care unit. Lastly, two, and no less than one feeling after COVID were present in 69,8 %, 39,7 %, and 23,2 % of cases, as well table 1.
|
Table 1. Post-COVID Symptom Duration (N = 186) |
||
|
Variables |
Frequency |
Percentage |
|
Duration (in months accomplished) |
||
|
< 51 |
166 |
81,1 |
|
51 to 58 |
12 |
6,6 |
|
≥61 |
10 |
3,5 |
|
Sex |
||
|
Male |
125 |
77,3 |
|
Female |
61 |
22,7 |
|
Comorbidity |
||
|
None |
115 |
51,7 |
|
Asthma |
38 |
28,6 |
|
Hypertension |
25 |
25,3 |
|
Diabetes |
12 |
6,3 |
|
Thyroid disease |
8 |
2,4 |
|
An ischemia heart problem |
4 |
2,3 |
|
Smoking status |
||
|
Non-smoker |
150 |
72,5 |
|
Current smoker |
27 |
24,6 |
|
The problem in the initial phase |
15 |
6,2 |
|
necessary hospitalisation |
40 |
21,6 |
|
Required ICU support |
5 |
2,8 |
|
Post-COVID symptoms |
||
|
a minimum of one indication |
128 |
58,7 |
|
Two or additional signs |
74 |
48,6 |
|
at least three signs |
45 |
32,3 |
Post-COVID symptoms and duration
Following acute phase, individuals stated that the majority of their symptoms after recovering from COVID-19 diminished within a period of thirty days. Fewsymptoms, such as weariness (7,2 %), breathing problems (5,4 %), lack of focus (3,7 %), hair loss (3,2 %), memory problems (2,3 %), sleep disruption (3,8 %), bone ache, too (2,5 %), however, remained for more than A period of 60 days, that remains even after the individual has completely recuperated are shown in table 2.
|
Table 2. Time span for post-acute COVID effects (N=186) |
||||
|
Post-COVID symptoms |
When the share-acute timing, permanence |
|||
|
Members’ recurrence a majority a |
||||
|
|
|
Abrupt post-COVID syndromes |
Prolonged after-COVID effects |
|
|
Total N=186 |
|
<30 days |
31-60 days |
> 60 days |
|
Pulmonary and cardiovascular |
||||
|
Having difficulty inhaling |
21 (8,4) |
5 (1,8) |
6 (1,1) |
10 (8,3) |
|
Cough |
10 (8,3) |
8 (3,6) |
4 (3,3) |
- |
|
Palpitation |
13(5,9) |
7 (6,8) |
4 (3,3) |
- |
|
Chest pain |
5 (2,7) |
5 (3,8) |
3 (0,6) |
3 (0,6) |
|
Rhinorrhea |
4 (1,1) |
4 (3,3) |
- |
- |
|
Throat irritation |
2 (0,5) |
3 (0,7) |
- |
- |
|
Neurological and psychiatric |
||||
|
Tiredness |
82 (41,0) |
57 (27,4) |
12(6,4) |
13 (7,1) |
|
Sleep disturbance |
23 (15,6) |
19 (7,4) |
3(0,6) |
5 (1,8) |
|
Lack of concentration |
20 (13,6) |
8(7,6) |
5 (3,8) |
11 (6,4) |
|
Memory lapses |
11 (6,0) |
6 (4,4) |
3 (0,7) |
6(2,5) |
|
Headache |
10 (3,5) |
10 (6,1) |
5 (3,8) |
3(0,3) |
|
Anosmia |
10(4,7) |
5 (1,6) |
6 (4,4) |
- |
|
Irritabilit |
6(2,5) |
4 (5,4) |
- |
2 (1,1) |
|
Loss of taste |
8(5,2) |
6 (4,4) |
3(0,7) |
3 (0,3) |
|
Depressed mood |
5 (4,83) |
1 (4,8) |
- |
- |
|
Anxiety |
5 (3,8) |
4 (3,3) |
- |
3 (0,7) |
|
Vertigo |
4 (3,3) |
4 (3,3) |
- |
- |
|
Gastrointestina |
||||
|
Loss of appetite |
9 (5,6) |
8 (5,4) |
- |
3 (0,7) |
|
Weight loss |
6(4,4) |
2 (4,4) |
- |
- |
|
Diarrhoea |
5 (3,6) |
5(3,8) |
- |
- |
|
Abdominal pain |
3(0,7) |
3(0,7) |
- |
- |
|
Nausea |
3 (0,7) |
- |
3 (0,7) |
- |
|
Musculoskeletal |
||||
|
Muscle pain |
14 (8,3) |
10(3,2) |
- |
- |
|
Joint pain |
6 (6,5) |
8 (4,9) |
- |
5 (3,4) |
|
Cutaneous |
||||
|
Hair fall |
11 (6,6) |
3 (0,8) |
- |
6 (2,5) |
|
Rash |
4(3,3) |
4 (3,3) |
- |
- |
Variables contributing to sustained post-COVID effects
Considering various topics, 43 (32,6 %) acknowledged having experienced at least one persistent COVID effect after. The modified linear regression model for any long-lasting indicators of COVID revealed that those who participated who were female were 3,88 times more likely than participants who were male to experience long post-COVID symptoms (OR, 3,68; 95 % CI, 2,37-5,05; p-value: 0,020). Persons with coexisting diseases were 2,28 times more possible than non-participants experience ongoing Subsequent symptoms (3,38; 95 % CI, 2,06-3,68; p: value, 0, 020). Compared to others, instances a higher possibility of persistent post-acute effects (OR, 3,36; 95 % CI, 2,07-4,79; 0, 020 as the significance level) table 3.
Number of patients with shock
A 49 of the participants reported experiencing at least one post-acute COVID-19 symptom, with extreme fatigue (36 %), dyspnea (21 %), neurocognitive challenges trouble concentrating, and “brain fog” (25 %), headaches (32 %), and joint pain (24 %) being the most prevalent (figure 1). Living in dread the effect of prolonged COVID on participants’ confusion life, obtaining GP care, and ways for enhanced services to promote recovery from long COVID were the four themes that arose from the interviews. The reported COVID-19 symptoms during the acute and post-acute phases are shown in figure 1.
|
Table 3. Determinants of prolonged post-COVID syndrome (N=186) |
||
|
Variables |
Long-Lasting Afterwards Sign |
|
|
Unadjusted Odds |
Adjusted Odds A |
|
|
Lifespan |
3,05 (0,96-1,08) |
3,05 (0,97-3,09) |
|
Gender |
||
|
Man |
Referent |
|
|
Woman |
4,48 (1,25-2,91)b |
4,77 (3,26-4,08)b |
|
Comorbidity |
||
|
Absent |
Referent |
|
|
Presented |
4,56 (3,27-8,18)c |
4,26 (3,06-2,77)b |
|
Previous cigarettes |
||
|
Smoke abstainer |
Referent |
|
|
Active smoker |
0,37 (0,13-1,42) |
0,64(0,18-4,36) |
|
A problem in the beginning |
||
|
No |
Referent |
|
|
Yes |
4,18 (0,68-4,96) |
4,8 (0, 609-9,283) |
|
Hospital admission |
||
|
No |
Referent |
|
|
Yes |
3,17 (0,55-4,73) |
3,06 (0,44-4,57) |
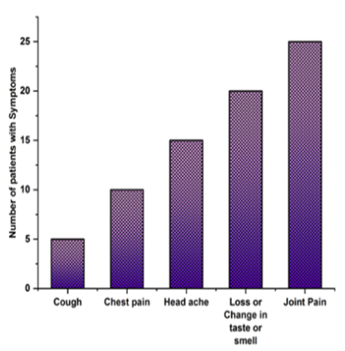
Figure 1. Acute and post-acute COVID-19 symptoms that were reported
DISCUSSION
According to our study, despite getting better after an illness, 24 % of those surveyed retained at least one sign for more than 60 days an acute illness, and 70 % of patients experienced effects after COVID. Discovered that 87 % COVID-19 hospitalized healthcare participant’s has residual issues, with 43 % having nearly 55 % of individuals experience has three following duration of 60 days after starting of problems. Similar to this, 66 % of patients still exhibited long-COVID symptoms 60 days later. In a multi-country investigation, found that roughly 32 % of the people with COVID-19 infection did not recover their prior state of health two to three weeks after their diagnosis. Numerous studies on viral infections, such as MERS and SARS, revealed respiration dysfunction, decreased exercise capacity, psychological issues like post-traumatic stress disorder (PTSD), long duration of six months, individuals can develop depression, anxiety, decline the overall quality of life. The condition persisted in CT findings during duration of seven years subsequent to SARS illness.
CONCLUSIONS
The goal of the research was to measure the post-COVID symptom problem and to prepare healthcare professionals for the upcoming load. Comorbid diseases and female sex are proven to be risk factors for long-lasting COVID symptoms. Counselling the patient about their illness will set expectations because the majority of patients had decreasing symptoms with time. Patients experiencing incapacitating symptoms, however, need to be continuously watched. On the basis of the results of the prospective research, programs for practical rehabilitative and psychiatric treatment need to be created.
REFERENCES
1. Rao, Kailing Adriel, et al. “Factors associated with mental health outcomes in emergency department healthcare workers on the frontlines of the COVID-19 pandemic.” Singapore Medical Journal 64.2 (2023): 141-145.
2. Sawant, Neena, et al. “Psychiatric sequelae and COVID experiences of post COVID-19 recovered resident doctors and interns of a Tertiary General Hospital in Mumbai.” J Assoc Physicians India 69.4 (2021): 22-26.
3. Boas, Hagai, and Nadav Davidovitch. “Into the “new normal”: The ethical and analytical challenge facing public health post-COVID-19.” International Journal of Environmental Research and Public Health 19.14 (2022): 8385.
4. Rahman, Fahad I., Md Rabiul Islam, and Mohiuddin A. Bhuiyan. “Mucormycosis or black fungus infection is a new scare in South Asian countries during the COVID‐19 pandemic: Associated risk factors and preventive measures.” Journal of Medical Virology 93.12 (2021): 6447.
5. Hill, Elaine, et al. “Risk factors associated with post-acute sequelae of sars-cov-2 in an ehr cohort: A national covid cohort collaborative (n3c) analysis as part of the nih recover program.” medRxiv (2022).
6. Lewandowska, Michalina, et al. “Impact of the COVID-19 pandemic on the dental service: A narrative review.” Dental and Medical Problems 58.4 (2021): 539-544.
7. Simons, Gemma, and David S. Baldwin. “A critical review of the definition of ‘wellbeing’for doctors and their patients in a post Covid-19 era.” International Journal of Social Psychiatry 67.8 (2021): 984-991.
8. Tang, PeiXi, and MaoSheng Lee. “Exploring the necessity of psychological rounds and psychological interventions in general hospitals in the post-COVID-19 period.” Frontiers in Psychology 13 (2022): 916776.
9. Fiala, Kenneth, Joshua Martens, and Alaa Abd-Elsayed. “Post-COVID pain syndromes.” Current pain and headache reports 26.5 (2022): 379-383.
10. Park, Jaeyoung, et al. “The COVID-19 pandemic response and its impact on post-corona health emergency and disaster risk management in Republic of Korea.” Sustainability 15.4 (2023): 3175.
11. Johnson, Stephanie B., and Frances Butcher. “Doctors during the COVID-19 pandemic: what are their duties and what is owed to them?.” Journal of Medical Ethics 47.1 (2021): 12-15.
12. Barca, Ida, et al. “Telemedicine in oral and maxillo-facial surgery: an effective alternative in post COVID-19 pandemic.” International journal of environmental research and public health 17.20 (2020): 7365.
13. Menges, Dominik, et al. “Burden of post-COVID-19 syndrome and implications for healthcare service planning: A population-based cohort study.” PloS one 16.7 (2021): e0254523.
14. Manchikanti, Laxmaiah, et al. “The impact of COVID-19 on interventional pain management practices is significant and long-lasting: an interventional pain management physician survey.” Pain Physician 25.2 (2022): 131.
15. Iyengar, Karthikeyan P., Vijay Kumar Jain, and Raju Vaishya. “Current situation with doctors and healthcare workers during COVID-19 pandemic in India.” Postgraduate medical journal 98.e2 (2022): e121-e122.
16. Deora, Harsh, et al. “Adapting neurosurgery practice during the COVID-19 pandemic in the Indian subcontinent.” World neurosurgery 142 (2020): e396-e406.
17. Sultana, Sarmin, et al. “Duration and risk factors of post-COVID symptoms following recovery among the medical doctors in Bangladesh.” Cureus 13.5 (2021).
18. Marin, Ruxandra-Cristina, et al. “Management of antiretroviral therapy with boosted protease inhibitors—darunavir/ritonavir or darunavir/cobicistat.” Biomedicines 9.3 (2021): 313.
19. Azam, Zaffar, et al. “Phytoconstituents as novel osteo-protective agents: Implications in bone health.” Frontiers in Bioscience-Landmark 25.7 (2020): 1259-1296.
20. Rajesh, N., and Prasanna Ranjith Christodoss. “Analysis of origin, risk factors influencing COVID-19 cases in India and its prediction using ensemble learning.” International Journal of System Assurance Engineering and Management (2021): 1-8.
FINANCING
None.
CONFLICT OF INTEREST
None.
AUTHORSHIP CONTRIBUTION
Conceptualization: Divya. V, Ioana Roxana Codru, Vasu Saini, Parthkumar Devmurari, Samaksh Goyal, Prabhjot Kaur.
Data curation: Divya. V, Ioana Roxana Codru, Vasu Saini, Parthkumar Devmurari, Samaksh Goyal, Prabhjot Kaur.
Formal analysis: Divya. V, Ioana Roxana Codru, Vasu Saini, Parthkumar Devmurari, Samaksh Goyal, Prabhjot Kaur.
Drafting - original draft: Divya. V, Ioana Roxana Codru, Vasu Saini, Parthkumar Devmurari, Samaksh Goyal, Prabhjot Kaur.
Writing - proofreading and editing: Divya. V, Ioana Roxana Codru, Vasu Saini, Parthkumar Devmurari, Samaksh Goyal, Prabhjot Kaur.