doi: 10.56294/saludcyt2024.586
REVIEW
Analysis of Trends in the Use of Artificial Intelligence in Diagnosis and Treatment
Análisis de las tendencias en el uso de la inteligencia artificial en el diagnóstico y el tratamiento
Vadim Pererva1 ![]() *, Dmytro Maltsev2
*, Dmytro Maltsev2 ![]() *, Oleksandr Hruzevskyi3
*, Oleksandr Hruzevskyi3 ![]() *, Leonid Gai4
*, Leonid Gai4 ![]() *, Yurii Dekhtiar5
*, Yurii Dekhtiar5 ![]() *
*
1Bogomolets National Medical University, Faculty of Dentistry, Dental Surgery, Kyiv, Ukraine.
2Bogomolets National Medical University, Experimental and Clinical Medicine Institute, Kyiv, Ukraine.
3Odessa National Medical University, Epidemiology and Biosafety Department with Course of Microbiology and Immunology, Odesa, Ukraine.
4National Medical University Traumatology and Ortopedy Department, Odesa, Ukraine.
5Odessa National Medical University, General and Military Surgery Department with Course of Urology, Odesa, Ukraine.
Cite as: Pererva V, Maltsev D, Hruzevskyi O, Gai L, Dekhtiar Y. Analysis of Trends in the Use of Artificial Intelligence in Diagnosis and Treatment. Salud, Ciencia y Tecnología. 2024; 4:.586. https://doi.org/10.56294/saludcyt2024.586
Submitted: 01-02-2024 Revised: 15-05-2024 Accepted: 21-09-2024 Published: 22-09-2024
Editor: Dr.
William Castillo-González ![]()
Corresponding author: Vadim Pererva *
ABSTRACT
Introduction: AI in healthcare has improved, making diagnostics more accurate and increasing the effectiveness of treatments. The present study discusses the AI trends in diagnostic and therapeutic applications and focuses on the presented practical applications and their effects on patient care. The purpose of this particular review is to focus on the current developments in the implementation of AI in the field of health care, present main use cases and successes, as well as discuss about the issues and concerns in the topic at hand.
Method: Previous studies on AI in healthcare with specific consideration of diagnostic image analysis and interpretation, histology and molecular pathology, whole-genome sequencing, and therapeutic decision support are discussed. The selection criteria included papers with data gathered from real-life AI cases and quantitative findings. Study materials were obtained from e-journals, conference papers, and established online sources with descriptive analysis being done on the data collected.
Results: a summary of the findings revealed a number of highly impactful subcategories focused on the use of artificial intelligence diagnostic imaging, especially in radiology, pathology, and genomics. The AI applications used in the fields of operations and drug discovery revealed the ability to accurately predict clinical trial outcomes and to create effective treatments.
Conclusion: first of all, AI can become a game changer in healthcare by enhancing diagnostics accuracy and treatment outcomes. The future research questions include further developing the methods that explain the AI models’ decisions, protecting the privacy of patient information, and reducing algorithmic bias for better fair healthcare for all. Therefore, better interactions between creators of AI and clinicians and regulatory authorities are pertinent to make sure that the full advantages of AI are realized in clinical practice to advance patient care.
Keywords: Machine Learning Algorithms; Pattern Recognition; Diagnostic Automation; Personalized Medicine; Ethical Aspects Of AI.
RESUMEN
Introducción: la IA en la atención sanitaria ha mejorado, haciendo que los diagnósticos sean más precisos y aumentando la eficacia de los tratamientos. El presente estudio analiza las tendencias de la IA en aplicaciones diagnósticas y terapéuticas y se centra en las aplicaciones prácticas presentadas y sus efectos en la atención al paciente.
Método: se analizan estudios previos sobre IA en la atención sanitaria con consideración específica del análisis e interpretación de imágenes diagnósticas, histología y patología molecular, secuenciación del genoma completo y apoyo a la toma de decisiones terapéuticas. Los criterios de selección incluyeron artículos con datos recogidos de casos reales de IA y resultados cuantitativos. Los materiales del estudio se obtuvieron de revistas electrónicas, ponencias de congresos y fuentes en línea establecidas, y se realizó un análisis descriptivo de los datos recopilados.
Resultados: un resumen de los resultados reveló una serie de subcategorías de gran impacto centradas en el uso de la inteligencia artificial para el diagnóstico por imagen, especialmente en radiología, patología y genómica. Las aplicaciones de IA utilizadas en los campos de las operaciones y el descubrimiento de fármacos revelaron la capacidad de predecir con precisión los resultados de los ensayos clínicos y de crear tratamientos eficaces.
Conclusiones: en primer lugar, la IA puede cambiar las reglas del juego en la atención sanitaria al mejorar la precisión de los diagnósticos y los resultados de los tratamientos. Las futuras cuestiones de investigación incluyen seguir desarrollando los métodos que explican las decisiones de los modelos de IA, proteger la privacidad de la información de los pacientes y reducir el sesgo algorítmico para una asistencia sanitaria más justa para todos. Por lo tanto, es pertinente mejorar la interacción entre los creadores de la IA y los médicos y las autoridades reguladoras para garantizar que se aprovechan todas las ventajas de la IA en la práctica clínica con el fin de mejorar la atención al paciente.
Palabras clave: Algoritmos de Aprendizaje Automático; Reconocimiento de Patrones; Automatización del Diagnóstico; Medicina Personalizada; Aspectos Éticos de la IA.
INTRODUCTION
Artificial intelligence simply called AI, has become one of the most impactful technologies in the modern world which has implications in almost every industry. (1,2) From these, the healthcare sector has been deemed as being the most promising area for the deployment of AI, with the capacity to improve the quality of patient care, and diagnostic results, as well as to optimize treatment delivery.(3) AI, in particular, is not just a disruption in the healthcare system, a shift in solutions, but is the dawn of an era revolutionizing the overall process of healthcare. AI in its simplest definition means the ability of a machine, especially a computer, to carry out tasks in a way that is associated with human intelligence.(4)
This includes the process of acquiring knowledge, that is, the information and the conditions for using this information, the learning process of drawing approximated or definite conclusions with the help of these conditions, and self-control.(5) Based on the functioning AI can be categorized into two major groups they are; The first one is narrow AI or weak AI which was created to perform a single specific task For instance, recognition of facial features or web search, and the second one is general AI which or strong AI which is an AI system that is capable of behaving intelligently in any field that a human being can.(6) AI technology emerged during the middle of the twentieth century with the primary source from the progress made in computer science, mathematics, psychology, and neuroscience.(7) You have likely worked with or at least used AI in the past decades, as AI has significantly developed through different phases such as rule-based systems, machine learning, and now deep learning.(8) Artificial intelligence has been subclassified into several categories of which the most famous is machine learning which is algorithms that are taught to look for patterns and make conclusions without being programmed to do so. Finally, there is deep learning, which is also a type of machine learning that applies neural networks with multiple layers; Deep learning is particularly useful in tasks that require soliciting, analyzing, and making sense of several features of data, especially images and voice.(9)
AI tools such as the machine learning, deep learning, natural language processing, and computer vision all increase healthcare operational performances. While CL is used to predict patient outcomes, detect disease at an early stage, and individualize treatments, there is no doubt about the superiority of DL in deciphering medical images that are often more accurate than human interpretation. NLP works with Clinical Notes and EHRs, streamlines documentation, and informs voice control, alleviating clerical loads. It allows for automatic diagnostics in medical picture analysis, which enhances efficiency. Nevertheless, and as shown from this analysis, difficulties such as the integration of the technology into existing processes, data protection, obtaining necessary approvals, and ethical issues persist and need to be approached for mainstream uptake.
To conclude, technologies like ML, DL, NLP, and computer vision are playing a significant role in improving the healthcare industry through optimization, increasing diagnostic accuracy, and even patient-centered care. ML is used for the assessment of patient status and risk scores, while DL shines in the medical image analysis outperforming even humans sometimes. NLP optimizes clinical documentation and helps voice-activated helpers to reduce the burden of health care professionals. Computer vision helps in particular, in automated image analysis, which makes the process faster and more accurate. However, issues like implementation into current routines, data protection issues, requirements for trials and approval, and various ethical issues still remain.
Therefore, there is a need for future research to address these challenges and to assess the potential of new applications of AI in healthcare. Better algorithms in artificial intelligence, better integration of the healthcare systems, and strong ethical frameworks will be crucial. Finally, the adoption of explainable AI to improve the levels of accountability and trust in AI will be important. As AI progresses, it seems that its impact on the healthcare industry will grow even more and bring benefits to patients as well as providers.
Current Trends in AI for Diagnosis
Diagnostic Imaging
AI Applications in Radiology
Radiotherapy is one of the major fields that is successfully augmented with the help of artificial intelligence to change the analysis and, in particular, the interpretation of medical images.(10) Currently, the most commonly used AI technique is Deep Learning and more specifically Convolutional Neural Networks in the field of radiology where AI applications are mainly used for analyzing various types of image data including X-rays, MRI, and CT scans. Such AI systems work on extraordinarily large datasets of medical images, and, thus, are capable of distinguishing the subtlest abnormalities.(11) In radiology, the use of AI has been made for different intentions such as to identify breakages, tumors, and other diseases. (12) For example, through intelligent systems, radiologists may prescreen images, and point out potential areas of interest which will help to shorten the time it would normally take for a scan to be analyzed or dismissed and decrease the rate of possible missed diagnoses.(13) Furthermore, AI can be utilized in calculating the size of tumors, observing the disease progression, and treatment planning, as it is difficult and time-consuming to perform manually.
|
Table 1. Describe the application of AI in radiology |
|
|
Application |
Description |
|
Image Interpretation |
AI algorithms analyze medical images (X-rays, CT scans, MRIs) to detect abnormalities such as tumors, fractures, or anomalies. |
|
Computer-Aided Diagnosis (CAD) |
AI assists radiologists in making diagnostic decisions by highlighting areas of concern or providing quantitative analysis. |
|
Image Reconstruction |
AI techniques improve image quality, reduce noise, or enhance specific features in radiographic images. |
|
Quantitative Image Analysis |
AI measures characteristics like tumor size, growth rate, or tissue density to aid in diagnosis and treatment planning. |
|
Predictive Analytics |
AI models predict patient outcomes or disease progression based on radiological data and patient history. |
|
Workflow Optimization |
AI automates routine tasks like image sorting, prioritization, and report generation, improving efficiency. |
|
Radiomics and Feature Extraction |
AI extracts quantitative features from images for deeper analysis, correlating imaging data with clinical outcomes. |
|
Quality Control |
AI monitors image quality during acquisition, flagging potential errors or artifacts for review. |
|
Education and Training |
AI simulates cases for training purposes, allowing radiologists to practice interpretation and decision-making. |
Accelerating Clinical Trials and Approvals
AI is also involved in a big way to fast-track clinical trials and drug approvals. This application focuses on patient’s particularities and can be used effectively in the recruitment and selection of patients for clinical trials. Another benefit is that it helps in estimating the patient response to the treatments being offered and assists in the most efficient trial designs to speed up the process of evaluation of the drugs regarding their efficacy and safety.(14) (figure 1,2)
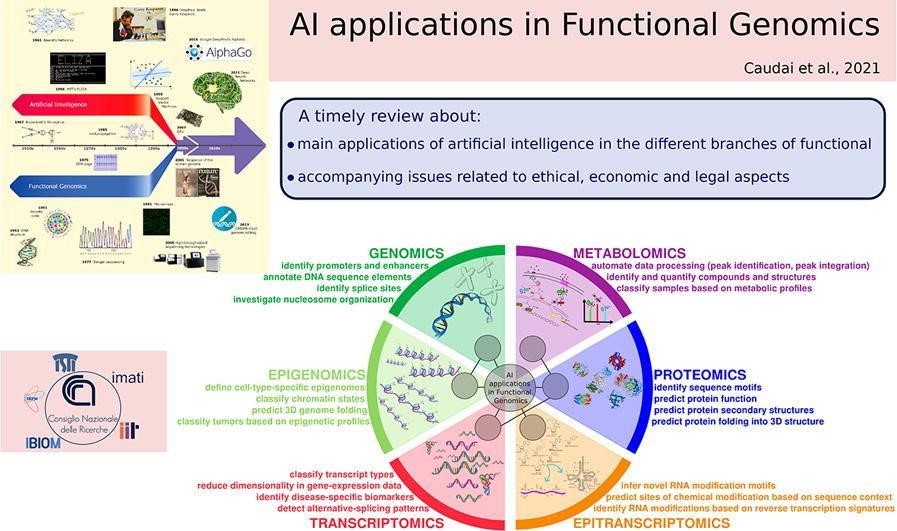
Figure 1. AI Innovations in Genetic Data Analysis (15)
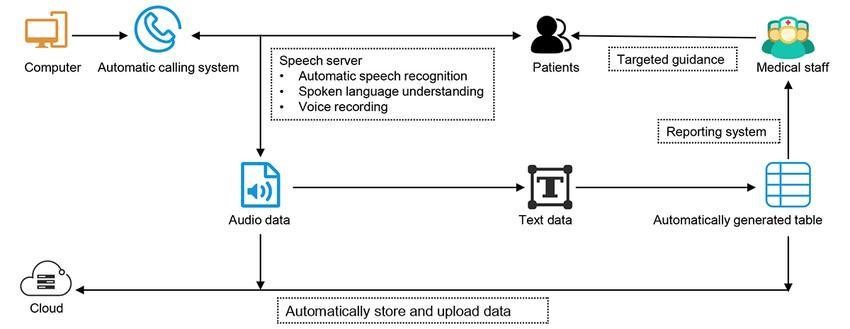
Figure 2. Comparative Outcomes in AI-Assisted Surgery
For example, the AI company Benevolent AI employs machine learning techniques to explore biomedical data for possible drug repurposing applications. In response to the emergence of COVID-19, Benevolent AI discovered that baricitinib, which is used to treat rheumatoid arthritis, may be useful in addressing COVID-19. From this, baricitinib was incorporated into clinical trials, which shows how AI can help in enhancing the speed at which a drug is developed.(16) (table 2).
|
Table 2. Summarizes the current trends in AI for the treatment |
||
|
Trend |
Description |
Examples |
|
Precision Medicine |
AI tailors treatments to individual patient profiles, improving efficacy and reducing side effects. |
AI-driven personalized cancer therapy plans. |
|
Robotic Surgery |
AI enhances surgical precision, reduces recovery times, and minimizes human error. |
AI-assisted laparoscopic surgeries, da Vinci Surgical System. |
|
Drug Discovery and Development |
AI accelerates the identification of new drug candidates and the optimization of clinical trials. |
AI models predicting drug interactions, AI for drug repurposing. |
|
AI in Treatment Planning |
AI optimizes treatment plans for various conditions, improving outcomes and efficiency. |
AI algorithms for radiotherapy planning in oncology. |
Research problem
Artificial intelligence (AI) has huge potential and its beneficial potential in healthcare cannot be overstated because AI can enhance diagnostic precision and treatment outcomes. However, despite the promise it holds, there are various challenges that limit the effectiveness of applying AI in clinical care. Some of the concerns include the following: The capability of AI systems to be interpreted, concerns to do with data protection, or the existence of prejudicial algorithmic inputs.
Research Focus
This narrative review specifically examined AI within the framework of healthcare where AI is used in diagnostic imaging, pathology, genomics, and treatment planning. Thus, the review seeks to establish how and to what extent the various AI technologies are being applied in the targeted fields and the results that the applications achieve as well as the emerging implementation issues.
Research Aim and Research questions
The purpose of this particular review is to focus on the current developments in the implementation of AI in the field of health care, present main use cases and successes, as well as discuss about the issues and concerns in the topic at hand. The review also seeks to give suggestions which may help in the future research and the possible ways of handling the noted challenges.
To achieve these objectives, the review addresses the following research questions:
1. In what areas of diagnostic imaging, pathology, genomics and treatment planning has AI been used?
2. What are the therapeutic benefits of use of AI within these contexts?
3. What problems are being encountered and what restrictions are experienced in the sphere of AI implementation in healthcare?
4. Which of these challenges can be addressed and how can broader use of AI in clinical applications be encouraged?
METHOD
General background
The integration of AI in healthcare is motivated to overcome several major critical challenges: the increasing service demand, medical data complexity, and diagnostic errors prevalence. AI technologies provide tools to help improve diagnosis and treatment accuracy while improving efficiency, leading ideally to improved patient outcomes.
Inclusion Criteria
The inclusion criteria for this review are as follows:
Study Type: Only articles published in peer-reviewed journals and only primary research on species, clinical trials, systematic review, and meta-analysis were considered.
Language: The articles were published in the international database in the English language.
Publication Date: Research papers that have been made available within the last two decades to make sure that the findings are up to date with the latest developments propelled by advanced technologies.
Exclusion Criteria
The exclusion criteria for this review are as follows:
Study Type: Systematic reviews and meta-analyses, clinical trials, and policies do not meet these criteria; excluded studies also included any that were conference abstracts, editorials or opinions, written in a letter or with letters between the authors.
Irrelevant outcomes: Literatures not focused on the main outcomes of this review.
Information Sources
The information sources for this review include: Databases such as PubMed, Google Scholar, IEEE Xplore, and ScienceDirect.
Data Collection
Data collection involved a systematic search of the specified databases using keywords such as “artificial intelligence,” “AI in diagnosis,” “AI in treatment,” “medical imaging AI,” “AI in genomics,” “AI in pathology,” “robotic surgery,” “precision medicine,” and “AI in healthcare.” The search was limited to articles published between 2000 and 2023. Titles and abstracts of retrieved articles were screened to assess their relevance to the review’s objectives.
A systematic search employing a specific search strategy yielded 800 articles initially. Subsequent screening based on titles and abstracts narrowed down the selection to 150 articles for full-text evaluation. Upon thorough assessment, 30 articles were deemed relevant and subsequently utilized to inform and construct this review (figure 3).
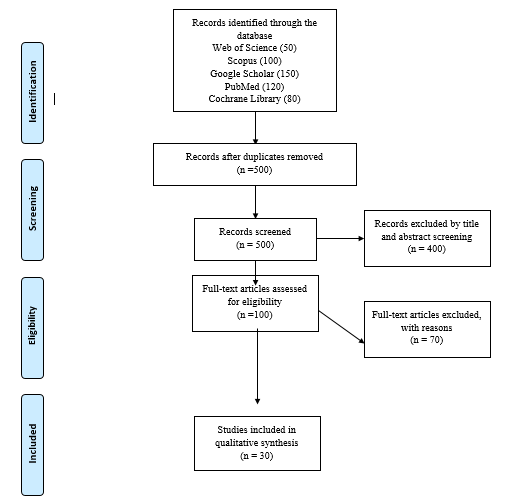
Figure 3. PRISMA flow diagram of the literature search
Descriptive Analysis
Qualitative data obtained from the included studies was synthesized using descriptive analysis. This entailed sorting the data according to certain themes including the use of AI in various sub-specialties in medicine, examples of effective AI solutions, and effects of AI on diagnostic and therapeutic outcomes. Thematic analysis facilitated the categorization of trends, successes, and challenges in the implementation of AI into healthcare systems.
RESULTS
A single-center randomized trial by Piette et al (17) enrolled 278 patients with chronic back pain from the Department of Veterans Affairs health system. They investigated the effectiveness of a personalized cognitive behavioral therapy for chronic pain (CBT-CP) program using AI and interactive voice response (IVR) technology compared to standard telephone CBT-CP. This was Clients in the AI-CBT-CP group completed daily feedback through IVR calls that the AI employed to personalize weekly therapy suggestions. These could encompass either a 45-minute or 15-minute therapist-delivered telephone session or an IVR-delivered message based on the participant’s preference. In the control group, the participants engaged in ten 45-minute telephone-administered CBT-CP sessions across 10 weeks conducted by a therapist. The target assessment was the Roland Morris Disability Questionnaire (RMDQ) at 3 and 6 months. This study demonstrated that the AI-CBT-CP participants had a 3-month mean difference of -0 in their RMDQ scores. change in SOB ranged from -2,06 to 0,62, 95 % CI: 72 points and 6 months difference of -1,24 points, 95 % CI, -2,48 to 0, compared with the standard CBT-CP group, and passed the criterion of noninferiority at both time points, P < 0,001 for both groups. Also, significantly more patients in the AI-CBT-CP group had clinically important gains in RMDQ scores after 6 months (37 % vs. 19 %; P = 0,01) and pain intensity (29 % vs. 17 %; P =. 03). Other secondary outcomes did not differ of any considerable ways: p-values lay around 0,05 which are not significant. More specifically, compared to the standard CBT-CP, the AI-CBT-CP program was found to be efficient as it used less than half of the therapist’s time.
Musculoskeletal symptoms including Neck and Shoulder pain/stiffness, and Low Back Pain are prevalent health conditions in the working population and are recognized as major causes of presenteeism. In the recent past, digital interventions have been applied to address the mentioned health issues; however, the efficiency of the interventions and their compliance rates are not very clear. Concerning the purpose of the Anan et al (18) study, the objective was to assess the change in musculoskeletal symptoms in workers who participated in the exercise-based AI interactive health promotion system implemented in the mobile message application. The expectation was that this program would enable people to stick to their exercise regimens. 150 patients with neck/shoulder stiffness/pain, low back pain, or both were enrolled in the study through e-mail invitations, randomized but unmasked. The intervention group participated in the AI health program in which a fax bot provided exercise guidelines daily in the LINE application for 12 weeks. The control group maintained their baseline level of care and treatment. The intensity of the reported neck/shoulder pain/stiffness and low back pain verbally and by self-administered web-based 1 to 5 scale at baseline, and after 12 weeks. The number of participants with conditions for inclusion in the study was 48 in the intervention group and 46 in the control group; the participants’ adherence rate was also high: 92 % (44/48) in the intervention group. There was a notable difference in the length of the intervention group’s neck/shoulder pain/stiffness and low back pain duration in comparison to the control group indicating a better prognosis (OR 6,36, 95 % CI 2).
Concerning AI in AF detection, a study involved 1003 patients with stroke risk factors and no known atrial fibrillation (AF), who wore a continuous ambulatory heart rhythm monitor for up to 30 days. The AI algorithm classified participants into high-risk and low-risk groups. AF was detected in 1,6 % of low-risk patients (6 out of 370) and 7,6 % of high-risk patients (48 out of 633), with high-risk patients having significantly higher odds of detection (odds ratio 4,98, 95 % CI 2,11-11,75, p=0,0002). AI-guided screening led to increased AF detection compared to usual care: In the end, each strategy is defined by the implementation of multiple related tactics that work in a coordinated manner. 3,6 % in the general population and 10,6 % in the high-risk group with AI screening versus 3,6 % with usual care: odds ratio 0,06, 95 % CI 0,04-0,07, p < 0,0001). 2,4 % in the low-risk group with AI screening versus 0,9 % in the normal low-risk group without AI (p=0,12). This indicates that the method of screening using AI increases the detection rate of completely asymptomatic AF.(19)
DISCUSSION
Research data also show increased sensitivity and specificity of AI in detection of the abnormalities with more accurate diagnosis. In pathology, AI has eliminated misdiagnosis and fastened the diagnosis procedure in histopathology, and biopsy. Regarding pathological data, otherwise time-consuming for doctors and resulting in possible misdiagnosis, thorough analysis can be done through AI tools hence drastically reducing the time required for diagnosis, especially in cancer detection. AI finds its relevant application in genomics particularly in the analysis of genetic data and in the synthesis of personalized medicine. Healthcare organizations use AI to analyze patients’ DNA to assess the risks of developing diseases, diagnose even the rarest genetic diseases, and organize targeted treatments due to the field of personalized medicine.(20) In precision medicine, the use of AI entails a way of delivering treatment that is unique to individual patients to enhance certain results and minimize toxic side effects. In oncology and managing chronic illnesses, AI applies patient statistics to identify the most suitable courses of action since multiple case studies support this claim. AI has played a significant role in the development of robotic surgery and the improvement of the robotic surgical instruments’ precision. This has contributed to increased efficiency in surgeries, faster healing, and reduced side effects. However, some of the difficulties persist with them including high costs and the need to have specialized personnel. AI has played a noteworthy role in enhancing drug discovery along with the identification of new candidates and the process of drug development.(21) Data gathered from biological sources can be fed into the algorithms to determine the efficiency and toxicity of likely drugs and consequently hasten clinical trial processes and regulatory approvals of the new drugs.
The scarcity of BC screening is tackled in this study by Wang et al (22) through designing and implementing a mobile phone-based Artificial Intelligence Infrared Thermography (AI-IRT) system for BC diagnosis. The study included a comprehensive, prospective clinical trial to determine the diagnostic accuracy of the AI-IRT system. For this purpose, two datasets and two models were developed, and internal and external validation and the comparison of diagnostic accuracy between AI models and clinicians were carried out. Participants in Dataset A included 2100 patients from 19 medical centers across nine regions of China. Dataset B for the independent external validation was collected from 102 patients of Langfang People’s Hospital. The binary model for differentiation between low-risk and intermediate to high-risk patients had an area under the ROC curve of 0,9487 (95 % CI: It was 0,9231-0,9744 in internal validation and 0,9120 (95 % CI: 0,8460-0,9790) in external validation. The accuracy of the binary model was higher than that of human readers for this text (0,8627 vs. 0,8088). Furthermore, the binary model proved to be superior to the multinomial model and used various diagnostic cut-off points depending on the BC risk for particular diagnostic objectives.
Concerning the AI use in orthopedic use the study investigated the effectiveness of using lumbar MRI images processed by an AI-enhanced U-net algorithm to evaluate the efficacy of chinkuei shin chewan decoction in treating lumbar spinal stenosis (LSS). The study involved 110 LSS patients divided into a control group and an experimental group, with the latter receiving the traditional medicine alongside the decoction. The AI-based U-net registration algorithm showed improved performance over the traditional U-net algorithm, with significantly reduced noise levels (P < 0,05) and higher Jaccard (0,84) and Dice (0,93) values compared to the traditional algorithm (J = 0,63, Dice = 0,81). Before treatment, the Oswestry Disability Index (ODI) scores were similar between the two groups. After treatment, both groups showed significant improvement in ODI scores, but the experimental group exhibited a more pronounced improvement (10,21 ± 5,05) compared to the control group (17,09 ± 5,23) (P < 0,05). The overall effective rates were 96,44 % for the experimental group and 82,47 % for the control group, with the experimental group significantly outperforming the control (P < 0,05). The diagnostic accuracy of lumbar MRI in the experimental group increased to 94,45 % with the AI algorithm, compared to 67,5 % before its introduction (P < 0,05).
The present blinded, randomized non-inferiority clinical trial aimed to compare the LVEF assessment skills of AI to sonographers in the first approach to a patient. The first aim of this study was the proportion of differences based on the primary endpoint, which was the change in LVEF from the initial and final assessment of AI or sonographer to the final cardiologist assessment when the LVEF change was more than 5 %.
He et al (23) scanned about 37,769 echocardiographic studies, 274 were excluded owing to the inadequate image quality based on the study. The statistical analysis of the results portrayed that 16,7 % in the control group have the following design features: intervention is implemented more intensively and on a larger number of subjects, the studies are randomized controlled trials, but the control group is less intensive and has fewer subjects. 2 % of the group of sonographers had significant changes revealing they were a difference of -10,4 % (95 % CI: Thus, prior AC administration significantly reduced the rate of infection by 13,2 % to 7,7 %, P < 0,001 for both non-inferiority and superiority. This indicated that the degree of correlation between the final cardiologist assessment of a patient and an independent previous cardiologist assessment was likely to be 6 mean absolute differences away from the true value. Today 29 % are in the AI group and only 7 % of the students are in the other group. 23 % in the sonographer group; representing -0,96 % (95 % CI: Enteral nutrition: mortality reduced from 34 % to -0,54 %, P < 0,001 for superiority. It also indicated that time was saved for both sonographers and cardiologists due to the AI-guided workflow while keeping the blinding because the cardiologists could not differentiate between the AI’s assessment and the sonographer’s assessment (Blinding index = 0,088). Therefore, AI is beneficial in the quantitative evaluation of LVEF as it is non-inferior and even superior to sonographers in the first assessment of LVEF. In the context of analysing trends in the use of artificial intelligence in diagnosis and treatment, it is important to note that Chalyy et al. (24) discuss the application of neutron and light spectroscopy in confined liquids, which could provide new diagnostic tests for tumour formation. In examining trends in the utilisation of artificial intelligence in the context of diagnosis and treatment, it is imperative to consider the physicochemical characteristics of MRI artefacts, as elucidated by Tsekhmister et al.(25)
CONCLUSION
This narrative review focuses on the increased application and progress of AI in diagnosing and managing several diseases. AI is different from the other methodologies as it creates significant progress in a short amount of time: applying it to diagnostics, imaging, pathology, genomics, and treatment planning, the performance increases in terms of accuracy and personalization while shortening the time required for the tasks. That is why the review highlights that AI can pave the way for the development of advanced methods of diagnostics, precise plans of treatment, and faster identification of new medications that will contribute to the improvement of patients’ conditions. Further study in this area is recommended to explore more applications of AI in clinical work fully. Future research in the application of AI in the healthcare sector should work to improve the understandability of the models to gain confidence in the professionals.
REFERENCES
1. Ossowska A, Kusiak A, Świetlik D. Artificial Intelligence in Dentistry-Narrative Review. Int J Environ Res Public Health. 2022;19(6). doi:10.3390/ijerph19063449
2. Gupta R, Srivastava D, Sahu M, Tiwari S, Ambasta RK, Kumar P. Artificial intelligence to deep learning: machine intelligence approach for drug discovery. Mol Divers. 2021;25(3):1315-1360. doi:10.1007/s11030-021-10217-3
3. Hamet P, Tremblay J. Artificial intelligence in medicine. Metabolism. 2017;69S:S36-S40. doi:10.1016/j.metabol.2017.01.011
4. Mintz Y, Brodie R. Introduction to artificial intelligence in medicine. Minim Invasive Ther Allied Technol. 2019;28(2):73-81. doi:10.1080/13645706.2019.1575882
5. Hashimoto DA, Witkowski E, Gao L, Meireles O, Rosman G. Artificial Intelligence in Anesthesiology: Current Techniques, Clinical Applications, and Limitations. Anesthesiology. 2020;132(2):379-394. doi:10.1097/ALN.0000000000002960
6. Itchhaporia D. Artificial intelligence in cardiology. Trends Cardiovasc Med. 2022;32(1):34-41. doi:10.1016/j.tcm.2020.11.007
7. Wang H, Fu T, Du Y, et al. Scientific discovery in the age of artificial intelligence. Nature. 2023;620(7972):47-60. doi:10.1038/s41586-023-06221-2
8. Chen M, Decary M. Artificial intelligence in healthcare: An essential guide for health leaders. Healthc Manag forum. 2020;33(1):10-18. doi:10.1177/0840470419873123
9. Nensa F, Demircioglu A, Rischpler C. Artificial Intelligence in Nuclear Medicine. J Nucl Med. 2019;60(Suppl 2):29S-37S. doi:10.2967/jnumed.118.220590
10. Bakhmat N, Krasnoshchok I, Voron O. International Experience of Using E-Learning during Pandemics and Military Conflicts. ELIJ [Internet]. 2023 Sep. 25 [cited 2024 Aug. 5];1(2):68-85. Available from: https://www.el-journal.org/index.php/journal/article/view/7
11. Sofilkanych N, Vesova O, Kaminskyy V, Kryvosheieva A. The impact of artificial intelligence on Ukrainian medicine: benefits and challenges for the future. FM [Internet]. 2023 Dec. 30 [cited 2024 Aug. 5];2(4):28-39. Available from: https://futurity-medicine.com/index.php/fm/article/view/56
12. Nikolenko K. Artificial Intelligence and Society: Pros and Cons of the Present, Future Prospects. FPH [Internet]. 2022 Jun. 30 [cited 2024 Aug. 5];1(2):54-67. Available from: https://futurity-philosophy.com/index.php/FPH/article/view/12
13. Zaitsev S. Using Digital Tools to Increase the Competitiveness of Small Businesses (Experience of Full-Service Bakeries). FSocS [Internet]. 2023 Dec. 20 [cited 2024 Aug. 5];1(4):75-90. Available from: https://futurity-social.com/index.php/journal/article/view/21
14. Vatansever S, Schlessinger A, Wacker D, et al. Artificial intelligence and machine learning-aided drug discovery in central nervous system diseases: State-of-the-arts and future directions. Med Res Rev. 2021;41(3):1427-1473. doi:10.1002/med.21764
15. Caudai C, Galizia A, Geraci F, et al. AI applications in functional genomics. Comput Struct Biotechnol J. 2021;19:5762-5790. doi:10.1016/j.csbj.2021.10.009
16. Mehta P, Titanji BK. Baricitinib in COVID-19: a coming-of-age from artificial intelligence to reducing mortality. Lancet (London, England). 2022;400(10349):338-339. doi:10.1016/S0140-6736(22)01295-8
17. Piette JD, Newman S, Krein SL, et al. Patient-Centered Pain Care Using Artificial Intelligence and Mobile Health Tools: A Randomized Comparative Effectiveness Trial. JAMA Intern Med. 2022;182(9):975-983. doi:10.1001/jamainternmed.2022.3178
18. Anan T, Kajiki S, Oka H, et al. Effects of an Artificial Intelligence-Assisted Health Program on Workers With Neck/Shoulder Pain/Stiffness and Low Back Pain: Randomized Controlled Trial. JMIR mHealth uHealth. 2021;9(9):e27535. doi:10.2196/27535
19. Noseworthy PA, Attia ZI, Behnken EM, et al. Artificial intelligence-guided screening for atrial fibrillation using electrocardiogram during sinus rhythm: a prospective non-randomised interventional trial. Lancet (London, England). 2022;400(10359):1206-1212. doi:10.1016/S0140-6736(22)01637-3
20. Jonas R, Earls J, Marques H, et al. Relationship of age, atherosclerosis and angiographic stenosis using artificial intelligence. Open Hear. 2021;8(2). doi:10.1136/openhrt-2021-001832
21. Ma M, Liu R, Wen C, et al. Predicting the molecular subtype of breast cancer and identifying interpretable imaging features using machine learning algorithms. Eur Radiol. 2022;32(3):1652-1662. doi:10.1007/s00330-021-08271-4
22. Wang X, Chou K, Zhang G, et al. Breast cancer pre-clinical screening using infrared thermography and artificial intelligence: a prospective, multicentre, diagnostic accuracy cohort study. Int J Surg. 2023;109(10):3021-3031. doi:10.1097/JS9.0000000000000594
23. He B, Kwan AC, Cho JH, et al. Blinded, randomized trial of sonographer versus AI cardiac function assessment. Nature. 2023;616(7957):520-524. doi:10.1038/s41586-023-05947-3
24. Chalyy KA, Bulavin LA, Chekhun VF, Chalyi AV, Tsekhmister YV, Chernenko LM. Fundamentals and medical applications of neutron and light spectroscopy of confined liquids. In: Dössel O, Schlegel WC, editors. World Congress on Medical Physics and Biomedical Engineering, September 7 - 12, 2009, Munich, Germany. IFMBE Proceedings, vol 25/13. Berlin, Heidelberg: Springer; 2009. https://doi.org/10.1007/978-3-642-03895-2_57.
25. Tsekhmister Y, Stepanenko V, Konovalova T, Tsekhmister B. Analysis of Physicochemical Natures of Modern Artifacts in MRI. Int. J. Onl. Eng. [Internet]. 2022 Mar. 8 [cited 2024 Aug. 9];18(03):pp. 89-100. Available from: https://online-journals.org/index.php/i-joe/article/view/25859
CONFLICTS OF INTEREST
None.
FINANCING
None.
AUTHORSHIP CONTRIBUTION
Conceptualization: Vadim Pererva, Dmytro Maltsev.
Data curation: Oleksandr Hruzevskyi.
Formal analysis: Dmytro Maltsev.
Research: Yurii Dekhtiar, Leonid Gai.
Methodology: Vadim Pererva, Yurii Dekhtiar.
Project administration: Dmytro Maltsev.
Resources: Oleksandr Hruzevskyi.
Software: Leonid Gai.
Supervision: Vadim Pererva.
Validation: Yurii Dekhtiar.
Display: Leonid Gai.
Writing – original draft: Dmytro Maltsev, Yurii Dekhtiar.
Writing – review and editing: Oleksandr Hruzevskyi.